Rehabilitation after surgery, stroke, or injury is most effective when the patient is a highly motivated participant. However, many physical therapists concede that engaging a patient is often a tough sell.
“Many medical procedures and treatments are done to a patient by a health care provider, and the patient’s role in the treatment is small,” said Karen Lohmann Siegel, a physical therapist at the National Institute of Health Clinical Center, in a recent institute newsletter. “That is not the case in rehabilitation. In rehab, the patients do a lot of the work themselves to get better.”
Indeed, studies have shown that poor patient participation in physical and occupational therapy has clinical implications that could lead to reduced functional improvement and longer lengths of stay. The good news is that a great deal of new and emerging technologies now hold the potential to motivate and keep patients engaged in their recovery.
Among these exciting developments are devices that utilize a range of technological advances, such as gaming, virtual reality, anti-gravity, robotics, and aquatics. Coinciding with these discoveries is the recent ramp-up of post-acute care services in skilled nursing facilities. Over the last decade, long term care providers have expanded their range of services to include post-acute rehabilitation care, spurred on by the opportunity to bridge the gap from facility to home.
Also driving the shift is the need to complement ever-shrinking and abysmal Medicaid payments. Between 2001 and 2010 the provision of physical, speech-language, and occupational therapy climbed for nursing facility residents by more than 10 percent, according to an analysis conducted by the American Health Care Association/National Center for Assisted Living. As of 2010, the number of skilled nursing facility residents receiving specialty rehab had reached 24.6 percent, the research showed.
Building A Better Rehab Unit
As providers have taken on this role, their need for tools of the trade has become more critical than ever. One tool that is sure to to induce the “wow” factor is a true space-age device known as the AlterG Anti-Gravity Treadmill. Derived from NASA technology, the AlterG helps users walk in a weightless or near-weightless environment.
According to Gabriel Griego, vice president of marketing for AlterG, the genesis of the engineering came from NASA scientists who developed gravity control technology so astronauts could train during space exploration. “AlterG harnesses the technology to deliver anti-gravity on earth,” he says.

First developed by a Stanford University engineer as a sports medicine application for training and conditioning, AlterG launched its first product in 2007.
Last year, the company released its M300 model, built with skilled nursing rehabilitation patients in mind. Today, nearly 30 of them are in use in skilled nursing facility rehab units across the country. Among its therapeutic benefits is its ability to improve endurance and strengthen muscles, increase muscle tissue mass and decrease age-related muscle atrophy, advance range of motion, and improve balance, says Griego.
System Advantages
AlterG’s unweighting technology “reduces impact and stress on the body…proportional to the amount of unweighting selected, while simultaneously natural gait mechanics and muscle-firing patterns are preserved,” the company’s literature says.
Peoplefirst Rehabilitation, a therapy staffing company owned by Kindred Healthcare, is piloting the AlterG in several facilities, as has Life Care Centers of America. Patients use the device by stepping into what looks like a pair of pants that are attached to the treadmill. Once on the treadmill, it appears that the patient is inside an inflated, air-filled chamber that envelopes the user from the waist down.
Megan Harper, outpatient rehab manager at Life Care Center of Littleton, Colo., has used AlterG for more than one year. She finds the technology to have many benefits for patients and therapists alike.
“Patients feel very supported in the device,” she says. “They feel like they can do things they couldn’t if they were standing on the floor.” Although the device looks like it could be a little difficult to get patients into, Harper says she’s been able to get everyone to use it.
Patients of all types—short-term rehab, outpatient, and even long term care—have utilized the AlterG at Harper’s facility, including a 100-year-old woman who had not been ambulatory for a long time. Compared with a harness-assisted treadmill system—in which a patient is suspended by a harness while walking on a treadmill—the AlterG appears to be a superior technology.
Robotics Rule
According to a 2010 review of advances in neurorehabilitation, published in the journal Stroke, several technological advances are ripe for clinical application. Among them is the use of robotics. According to the review’s authors, some studies suggest that robot-assisted therapy can be effective for stroke rehab patients when compared with standard rehab therapy.
Andrew Butler, a neuroscience researcher and physical therapist in the School of Medicine at Emory University in Atlanta, specializes in upper body, post-stroke rehabilitation. Much of his research entails the use of a robotic device that improves hand movement in stroke survivors. The technology is available in two products—the Hand Mentor and the Foot Mentor—both created by Kinetic Muscles (KMI), in Tempe, Ariz.
According to Grant Farrell, KMI’s chief executive officer, the devices help users “maximize their potential for intensive neuro-rehab by using a robotic device combined with telemedicine.”
The product is used in nursing facilities, but was designed principally for use by patients undergoing rehabilitation in their own homes. The Hand Mentor includes an interactive training program that encourages patients to improve their hand functions.
Listed with the U.S. Food and Drug Administration (FDA) as a Class One medical device, the Hand Mentor’s technology was shown in clinical trials to be “an effective alternative or adjunct to the delivery of intensive task practice interventions to enhance hand function recovery in patients with stroke.”
Farrell notes that the Hand Mentor actively involves patients in their own rehabilitation by encouraging self-powered motion of the wrist and fingers and assisting movement when necessary.
How It Works
The devices themselves provide instructions and assistance by encouraging and challenging patients to achieve, surpass, and increase their goals using three types of visual feedback: force, position, and electrical activity of the muscle.
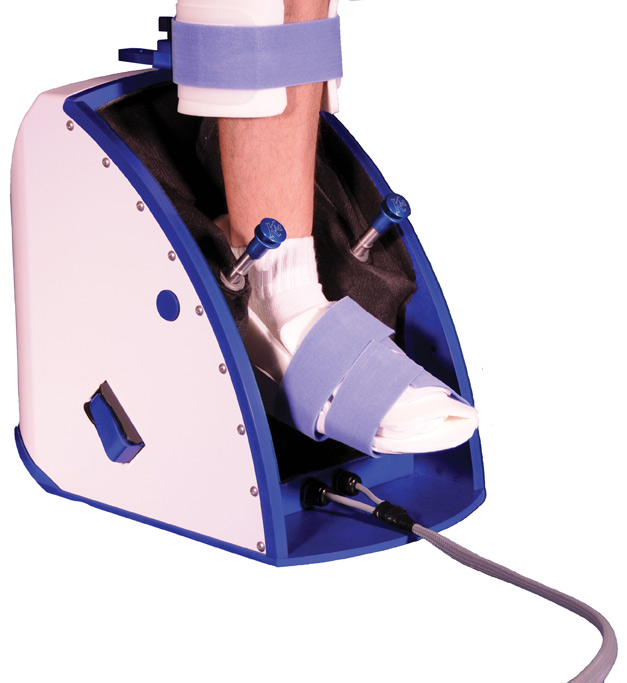
One of the most common impairments following stroke is the inability to extend the wrist and fingers. The Hand Mentor works by helping people with movement limitations relearn how to extend their wrist and fingers. It works like this: An “air muscle” pulls the linkage mechanism, assisting the patient with desired movement when the patient is not able to move her wrist or fingers on her own. An air muscle is a soft and springy air-driven actuator that pulls a linkage system that raises the hand and wrist in a fluid motion.
According to KMI’s website, the soft springy muscle-like properties of the “air muscle” make it safer than a motor- and gear-driven apparatus.
Stroke and other brain-injury patients of varying degrees of ability can benefit from stroke devices aimed at restoring wrist and finger movement. Patients with high tone or spasticity can increase their passive range of motion using one of KMI’s spasticity reduction programs. Patients with some movement capabilities can improve active range of motion with the motor control and active recruitment programs.
Butler, who has conducted research on the Hand Mentor for the past five years and continues to use the robotic mechanism in his current research, says he is testing a modality that combines a guided visual imagery treatment with the robotic device in an effort to help patients visualize the movement before they actually begin the work.
“For example, Tiger Woods visualizes his actions before he swings the golf club,” says Butler. “There’s evidence that a post-stroke patient who visualizes moving his hand before actually doing it improves the outcome and speeds up the process by increasing the number of repetitions a person performs without becoming fatigued.”
Evolution Of Virtual Reality
The Stroke review also examined the use of virtual reality and gaming. In a randomized, single-blinded clinical trial using the Nintendo Wii system versus recreational therapy, such as playing cards, bingo, or Jenga, the nine users of virtual reality “significantly improved in mean motor function,” researchers said, concluding that “virtual reality using the Nintendo Wii is a potentially effective alternative to facilitate rehabilitation therapy and promote motor recovery after stroke.”
Another study in the journal Physical Therapy revealed that the use of virtual reality by patients resulted in a “powerful effect” on the progress of cardiac rehabilitation. The study’s authors suggested that “incorporating virtual reality into rehabilitation programs will accelerate the maximum recovery of a patient’s cardiovascular fitness.”
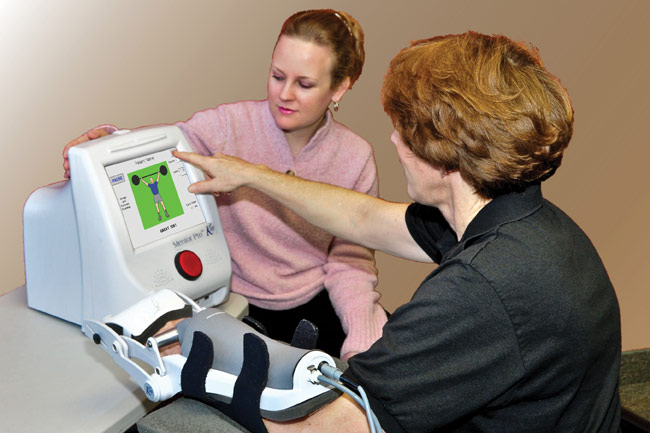
Although many rehab units deploy the Nintendo Wii system, it is not the only virtual reality game in town for use in rehab treatment. Accelerated Care Plus (ACP), a Reno, Nev.-based company that provides education and equipment to skilled nursing facilities, recently launched a virtual reality product geared specifically to rehabilitation.
Mark Richards, a physical therapist and ACP’s vice president of clinical education, says the new OmniVR system “automatically captures a patient’s image and creates a three-dimensional avatar of the patient.”
The patient views a large flat-screen color monitor and performs therapy-specific exercises and activities without the use of a controller. “The technology enables even very low-functioning patients to participate,” Richards says, noting that patients become quickly engrossed in the virtual world and therefore conduct a higher volume of exercise at a more intensive level.
While the Wii systems are widely used in rehabilitation, they are game-based, more focused on entertainment, and not always appropriate for lower-functioning elderly patients, says Richards. “They’re typically rapidly paced, visually intense, and intimidating to many patients.”
The OmniVR has multiple exercises, and each contains adjustable parameters to match the level of difficulty to each patient’s functional level. “This customization allows therapists to treat patients more effectively and better demonstrates the skills involved with virtual-reality-based therapy services.”
Richards views the OmniVR as an adjunct to traditional therapy. “Research demonstrates that therapy augmented with virtual reality may achieve better clinical outcomes.” What’s more, he says, studies have demonstrated that skills acquired in a virtual world transfer to real-world activity. The system is more costly than a Nintendo Wii, but Richards believes the OmniVR is superior because it is customized to the rehab world and in the near future will contain extensive standardized outcome measures such as gait, balance, and range of motion.
Charting Results
At Marquis Care at Mt. Tabor in Portland, Ore., the new technology is already earning high marks.
The systems being tested offer six different rehabilitation programs appropriate for a spectrum of aging adults from very frail to independent.
“As a way to prepare Marquis for the future, our management team has been working together to explore the ways health care might evolve over the next 20 years. Our guess is that technologies like the OmniVR will be at the forefront of that evolution,” said Phil Fogg Jr., Marquis Companies’ chief executive officer, in a statement.
In testing the OmniVR, the rehabilitation staff at Mt. Tabor worked with a patient who found it difficult to sit up on the side of the bed to get dressed, but once she immersed herself in a game on the OmniVR system that required her to lean side to side, staff members saw that the patient was able to balance on the edge of her bed, and her skills improved so much that she was able to put on a shirt without help.
According to ACP, in another game, a stroke patient used the upper part of his body to catch objects from side to side on the screen. Mt. Tabor staff were able to identify a significant deficit in the patient’s visual field and focus further therapeutic attentions to improving that deficit.
“We have already had several breakthrough moments with residents who were afraid to move, side step, or walk backwards, getting so caught up in the virtual games that they were moving in all directions without fear and with a large smile on their faces,” says Allison Dehaan, Mt. Tabor’s rehab director. “The most exciting piece is that these skills are transferred into their daily activities.”
Hydrotherapy Advancements
The use of water in rehab therapy is not new, but combining a treadmill with a moveable floor that is immersed in a pool is an innovative concept that is gaining ground in a wide variety of rehab treatment programs.
HydroWorx International, Middletown, Pa., produces hydrotherapy devices that combine treadmill training and the weightlessness of a pool. HydroWorx’s technology eliminates 20 percent to 100 percent of a person’s body weight, according to the company’s website. As a result, patients who are unable to exercise on land can achieve immediate rehabilitative results while carrying as little as 0 percent of their body weight under water.
In addition, hydrostatic pressure, water temperature, and resistance combine to enhance cardiovascular stamina, muscle strength, and flexibility and drive early range-of-motion gains during rehab.
Its key feature is gait training in a low-impact environment, which allows for “earlier replication of proper ambulatory biomechanics and reduces the accumulated damage of land exercise,” the website says.
HydroWorx’s most recent product line is the HydroWorx 2000 Series, which includes a moveable floor, an eight-foot by 12-foot underwater treadmill, resistance jet technology, and computer and camera systems. A Texas A&M study found that the results were significant and that the study participants improved their overall health and fitness in the HydroWorx pool without the joint trauma and “wear and tear” that one normally experiences working out on land.
Hydrotherapy research experiments at the University of Idaho also found that the HydroWorx pool can create “a metabolic and cardiovascular environment as stressful as traditional land-based treadmills but with reduced joint stress—a hallmark feature of aquatic therapy.”
In follow-up studies, positive results were also verified with factors such as maximal oxygen consumption, heart rate, ventilation, blood lactate, leg-stride rate and length, and perception of effort. According to HydroWorx, each study confirmed the effectiveness and equivalent responses with aquatic therapy versus land-based treadmills.
A Balancing Act
For Mary Van de Kamp, senior vice president of clinical operations for Peoplefirst, staying on top of advancements in technology and engineering is a key component of an effective rehab therapy program.
And given the variety of Medicare patients treated in rehab units today, it can be a tricky thing.
“When you have patients who are so medically complex, managing their care can be a balance between providing modalities they are most comfortable with and still are effective,” she says. “Younger patients, for example, are more comfortable with more high-tech devices that are used in rehab treatment, while older patients may not feel at ease with it.
“The balance is difficult because the technology also changes in a short amount of time.”
This can mean a higher cost for the facility as it scrambles to purchase the best, state-of-the-art equipment.
Nonetheless, the company stays abreast of the latest technology and engineering marvels that promise to send rehab residents home sooner.
Basics Work Best
Butler, the researcher, concedes that all the technological advances out there cannot replace the tried-and-true basics of movement and repetition. Physical exercise and hard work is a “magic pill” for successful physical rehabilitation, he says.
If so, then why bother with research? “I am focused on increasing the recovery curve,” says Butler.
“If we can develop therapies that reduce a patient’s stay in the hospital (or rehabilitation unit) from 20 days to seven days, and return them back to more activities of daily living,” all parties win, he notes. At the end of the day, the best rehabilitation therapy is not technology or engineering that will make stroke survivors better, says Butler. It’s people.
“If you can get the best people, the best doctors, nurses, and therapists who are the most qualified, and who have a passion and commitment to helping people,” that’s half the battle, he says.