States Caught In Funding Vise
2/1/2012
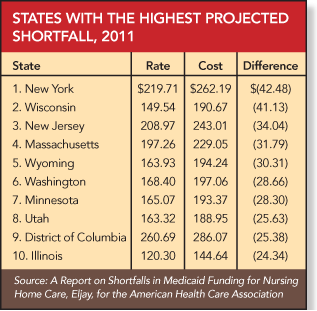
In New York state, which had the top-ranked deficit of $42.48 per Medicaid patient day, some providers are “hanging on by their fingernails” and have collaborated with unions to put multi-year labor contracts in suspension, said Richard Herrick, president and chief executive officer of the New York State Health Facilities Association. To close a $15 billion budget gap, the state has imposed a two-year global spending cap on Medicaid, in addition to a 2 percent across-the-board rate cut, said Herrick, who participated in a recent teleconference.
Nursing facilities mitigated the reduction somewhat by negotiating with the state for an alternative in the form of an additional 0.8 percent nonreimbursable assessment on nursing facilities. The assessment is a straight tax hike, separate and apart from the Medicaid provider tax program.
This alternative to the 2 percent cut yields equivalent savings for the state without burdening providers with the full force of the rate reduction.
In Wisconsin, where the Medicaid deficit is the second-highest in the nation, at $41.13 per patient day, providers have been working with the state “to remove a lot of inequities in the payment system” and “make the Medicaid program financially sustainable,” said Thomas Moore, executive director of the Wisconsin Health Care Association, who also participated in the teleconference. “Medicare cuts out of Washington have handicapped our efforts,” Moore said.
“The numbers speak for themselves,” he added. What the numbers don’t capture is the “human impact of the failings of Medicare and Medicaid to recognize what it costs to take care of the nation’s elderly.”