It’s always entertaining to watch old TV shows where hospitals and other health care facilities look very different than they do today. Nurses often wear caps and uniforms, the equipment looks very outdated—even primitive, there’s nary a computer in sight—and in the earliest programs, some practitioners are even smoking cigarettes in the exam room.
But one difference that points to a trend affecting long term and post-acute care (LT/PAC) centers is the amount of time patients spend in the hospital. Gone are the days where patients linger in hospital beds. As acute care stays are getting shorter, skilled nursing care centers are receiving patients “sicker and sooner” than ever before, and they face the challenge of gearing up to care for a more complex population.
Preparing to accept and manage these patients is challenging but not optional, says Mark McKenzie, chief executive officer of Focused Post-Acute Care Partners in Texas. “You need to do this or get out of business,” he says bluntly. “We are not the nursing centers of the ’80s, ’90s, or even 2005. Our patients are critically ill with many comorbidities. If you aren’t capable of managing that transition, you won’t be able to keep your doors open. Those are the only type of patients coming to skilled nursing.”
Rich Feifer, MD, chief medical officer at Genesis HealthCare Corp., agrees. “We are in an environment where you can’t cherry pick,” he says. “Everyone is looking for responsible, responsive partners who are willing to take a blend of cases. You can’t expect just to take the easy cases anymore.”
A Growing Concern
According to the U.S. Centers for Disease Control & Prevention, the average hospital inpatient length of stay was five days in 1999, down from 7.3 in 1980. The hospitalization rate dropped nearly 30 percent between 1980 and 1990. Between 1990 and 1999, the discharge rate dropped for patients between the ages of 15 and 64 but rose 11 percent for those 65 and older.
The average length of stay for surgeries that are common in older populations—such as hip replacements—have decreased. And at least one study from the University of Colorado in Aurora has suggested that a shorter length of hospital stay is associated with earlier readmission and that shorter hospital stays for elders may be detrimental. This isn’t just an American issue. In Australia, a survey found that nearly three-quarters of general practitioners say their patients had been discharged prematurely or inappropriately. Nearly 70 percent say it was more common than five years ago for patients to be discharged prematurely and inappropriately, and nearly 60 percent say they often found the discharge summary was inadequate or absent.
Clint Maun, senior partner and president of Maun-Lemke Speaking and Consulting in Nebraska, agrees, saying, “If you are known as a ‘cherry picker,’ you are useless to the hospital.”
 JoAnne Reifsnyder, PhD, MBA, MSN, FAAN, executive vice president of clinical operations at Genesis, adds, “There is no question we are seeing very different patients than we did even six or seven years ago.”
JoAnne Reifsnyder, PhD, MBA, MSN, FAAN, executive vice president of clinical operations at Genesis, adds, “There is no question we are seeing very different patients than we did even six or seven years ago.”
She says that those with an uncomplicated course—routine hip and knee replacements, for example—are going home or to rehab centers, and not to skilled nursing facilities, after the hospital. Instead, she says, “We are seeing those individuals with complex, chronic illnesses such as patients with heart failure who also have other comorbidities.”
Red, Yellow, Green
Gearing up to take sicker patients requires time and effort, but it is doable, and many organizations are finding success in this arena. It starts with a self-assessment and market analysis, McKenzie says, “working with the center office and regional and facility-based teams, who look at their strengths and weaknesses—focusing on what kinds of patients they are best equipped to care for. We look at each community and take it to a granular level.
“We focus on what they have now and what issues the communities view themselves as experts on,” he says. “Based on the skill sets they have, they are able to take specific kinds of patients, and every facility is unique—facility A takes these patients, facility B takes others. We don’t expect any facility to be everything to everyone, but we expect them to be extraordinarily competent at what they do.”
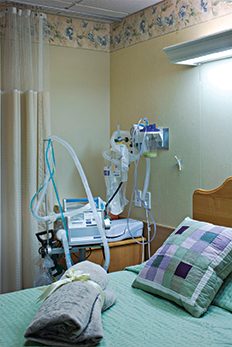
It also is important, says Maun, to consider the needs of area hospitals. For instance, he says, “If a hospital has patients on ventilators or trachs [tracheostomy tubes], you need to determine what you need to be able to accommodate these patients.” He adds, “Look at what is happening in your hospitals; look at their DRG [Diagnosis Related Group] codes. Use meetings and data research to move your facility to those levels.”
Kimberly Vermilyea, RN, BSN, NHA, MBA/MHCM, chief operating officer, post-acute segment, at Signature HealthCare, says, “We formulated a workgroup to delineate where opportunities present themselves in the industry and what hospitals are asking for.”
 Once facilities have a handle on what their capabilities are, says McKenzie, each potential admit is assessed via red, yellow, and green cards, based on the provider’s capabilities.” Green means the patient is accepted immediately—no questions. Yellow means the patient will be accepted but there is something unique about the person that requires special attention (such as equipment that needs to be purchased or leased). Red means the provider’s team “just doesn’t have the skill set to care for that patient.”
Once facilities have a handle on what their capabilities are, says McKenzie, each potential admit is assessed via red, yellow, and green cards, based on the provider’s capabilities.” Green means the patient is accepted immediately—no questions. Yellow means the patient will be accepted but there is something unique about the person that requires special attention (such as equipment that needs to be purchased or leased). Red means the provider’s team “just doesn’t have the skill set to care for that patient.”
However, McKenzie says, “Providers should be looking at how they can turn ‘red’ patients to ‘yellow’ and ‘yellow’ to ‘green.’” Specifically, this means looking at what additional investments in equipment, staffing, or other capital might enable the provider to care for specific types of conditions or illnesses. “The goal should be to limit the ‘red,’” he says.
“You have to start with the basics and move your way up,” Maun says. He suggests setting targets and identifying strategies to reach them. “You want to go from, say, 27 illnesses or conditions you won’t take to 24, then 20. You eventually want to get down to just four or five you won’t take.” To whittle down the list, providers need to determine staffing, training, equipment, and other additions or changes necessary to effectively manage these conditions.
“You don’t just want to accept more conditions and patients,” says Maun; “You want to do it quick.” This means having staff with knowledge, information, and training to be able to make fast, appropriate decisions about whether or not they can safely accept any given patient.
“If you’re not speeding up your decision making and your ability to make decisions, you won’t stay in the game,” Maun says. “You can’t just get into your networks; you have to prove yourself to stay there.”
Being agile and alert is essential to stay at the top of one’s high-acuity game, says Vermilyea. “You never know what will happen in the market. You need to do your research and keep your eye on trends.”
For example, she says, “When we started, the opioid crisis hadn’t yet hit, but we now are seeing more opioid dependency in our referrals from hospitals, so we decided that we need to be able to formulate some specialized training to manage it.” Team leaders should stay involved in their professional organizations as one way to keep a finger on the pulse of issues and trends, she says.
Niches, Transitional Units
It is important to develop niches, says Daniel Mendelson, MD, Konar Professor of Geriatrics and Palliative Medicine at the University of Rochester in New York and past chair of the American Hospital Association’s Section for Long-Term Care and Rehabilitation.
 Mendelson agrees that assessing strengths can show what niches are immediately good fits for the facility. For example, he says, “If you are good at dementia care, a neurobehavioral unit for difficult behaviors might be a good fit.” It also is worth developing competencies that the center is not currently strong in, he says, particularly if there is a need for them in the area.
Mendelson agrees that assessing strengths can show what niches are immediately good fits for the facility. For example, he says, “If you are good at dementia care, a neurobehavioral unit for difficult behaviors might be a good fit.” It also is worth developing competencies that the center is not currently strong in, he says, particularly if there is a need for them in the area.
“One facility here developed a niche regarding negative pressure wound treatment because others weren’t doing it. IV [intravenous] fluids and antibiotics are always in demand, so doing these are advantageous. And it’s relatively easy to develop policies and procedures and competencies around them.”
One way to focus on the special needs of higher-acuity patients is to create specialty transitional units. These, says Reifsnyder, “allow you to concentrate services on a separate unit” with social workers, therapists, nursing staff, and others devoted to safely and effectively manage patients without having them bounce back to the hospital or to the post-acute or long term care center once they return home.
These transitional units are essential, says Maun. “You can’t mix these patients with your long-term residents. You need these mini rapid-recovery transitional care units where you can apply focused training, documentation, and therapy coordination.” He suggests having people qualified by interview for the units.
“We put ‘Navy Seal Team 6’ level staffing in place. These have to be people who have the competence and confidence to efficiently and effectively manage the special needs of these patients.”
Checklists for Change
While a provider is examining what high-acuity conditions it is equipped to care for, it can be helpful to develop checklists of the equipment, technology, and other capabilities the team will need. Then they can match them to what each facility already has in place and what additions or modifications may be necessary. For example, McKenzie says, “We develop an equipment list. Then we acquire the capital, and we bring in team members for training, education, and certifications.”
Checklists, protocols, and policies and procedures will help ensure that staff are prepared and that there are no surprises. This is essential, as there is little room for surprises with high-acuity patients, he says.
Virginia-based geriatrician Jonathan Evans, MD, CMD, says, “It is critically important that you understand the care needs of any patient you accept. The consequences of not doing that are great and increase the likelihood that the patient will be readmitted to the hospital. You have to plan ahead for success.”
Preparing Staff
Taking higher-acuity patients represents a change from traditional nursing center care models, and staff need to be willing to make the necessary adjustments. Maun notes that it is essential to get team leaders, particularly the director of nursing (DON) on board.
“They need to realize that it’s all about value. If you help the DON see that they will be able to bring in extra nursing staff, enhance training, and have money for pay raises, you are more likely to get them on board,” he says.
“People are motivated to make changes based on the desire for ‘pain reduction.’ If you can help your team to understand how taking higher-acuity patients and establishing transitional units will decrease their pain and not increase their burdens, they are more likely to be willing to change.”
 Education and training are key to ensuring staff have the competence and confidence to handle higher-acuity patients. “We implement ongoing education on key topics such as IVs, wounds, congestive heart failure, etc.,” says McKenzie. “We start at the nursing level, and we bring in ancillary team members—such as social workers and therapists—and ensure that they have the training and knowledge they need to work with specialized populations,” he says.
Education and training are key to ensuring staff have the competence and confidence to handle higher-acuity patients. “We implement ongoing education on key topics such as IVs, wounds, congestive heart failure, etc.,” says McKenzie. “We start at the nursing level, and we bring in ancillary team members—such as social workers and therapists—and ensure that they have the training and knowledge they need to work with specialized populations,” he says.
Vermilyea says education needs to be ongoing, even for experienced nursing staff. “I often find that nurses lose their skill sets if they don’t use them regularly. So we need to make sure that their skills are current.”
In addition to ensuring adequate nursing staff, Mendelson says, “We have invested in a closed staffing model and professional medical directors. We have medical directors interface with hospitals so there is someone skilled and respected acting as a go-between. We also have advance practice providers and medical staff on site.”
Partnerships also are key, Mendelson says. “We partner with other nursing centers in the area. When patients are more stable, we will transfer them to a more traditional nursing center so that we can take more high-acuity patients. We bring all the pieces to the table to help give our team confidence.”
For example, Focused Post-Acute Care Partners has a wellness program to help sicker patients compensate for their deficits and disabilities. This, he says, has had a powerful impact on late-loss activities of daily living scores.
McKenzie notes that the company tries to make it an honor to work in a transitional unit. However, it is vital that staff on these units are comfortable working in this environment, which not only requires special skill sets but also may be more fast-paced and stressful, he says. Those who prefer working with long-term patients in a more traditional nursing center setting should not be pushed to work in special high-acuity units.
However, once a company has set its course toward higher-acuity patients, there may not be a place for staff who are unwilling or unable to change, Maun says.
“You have to find out why team leaders are hesitant to accept patients and identify how you increase their confidence and willingness to make it happen,” McKenzie says. Sometimes it may be necessary to change out leadership and move staff around if they continue to be unwilling to embrace the new model, he says.
“We don’t discard DONs and team leaders, but they need to get over this hump to succeed in this business moving forward.”
Smooth Transitions
“One of the biggest things for providers is access to information that ensures smooth transitions,” Mendelson says. “You need access to patient information before they leave the hospital and throughout the continuum. Anything you can do to streamline access to information and help with information gathering will make practitioners happier and help ensure the nursing center is prepared to care for the patient.”
“We try to formulate what the patient will need prior to admission,” says Vermilyea. “We have transitions-of-care nurses who get information from the hospital.” As a result, they know what equipment and services they will need to follow the patient through the skilled nursing center stay and when they eventually return to their home or long term care center in the community.
Finding the Proper Niches
Studying local supply and demand will help providers determine what high-acuity niches might be a good fiscal fit.
“In the Rochester area, with a new unit opening soon, there will be enough ventilator beds, so it wouldn’t be beneficial for another nursing center to take it on. However, there is a demand for IV antibiotics and dialysis, so those would be good areas to develop business plans and skill sets for,” says Mendelson.
“You need a plan that is sustainable and financially viable. You need to have finance and administrative people who understand payment structures and can do an accurate analysis.”
There is a risk associated with higher-acuity patients, but the best way to address it is to ensure and document that staff have the training and expertise as well as sufficient time to care for them.
As Alan Horowitz, RN, a health care attorney with Arnall Golden Gregory, explains, “The overarching issues facilities should consider when evaluating potential admissions is whether they have adequate personnel with the appropriate levels of expertise to manage care for those patients.”
 For instance, if a hospital wants to send a patient on a ventilator, he says, “you need to have respiratory therapists and nurses experienced in caring for individuals who require mechanical ventilation, as well as staff who can manage the equipment and safely perform related skills, such as changing tracheostomy tubes, providing tracheostomy care, and suctioning a resident’s trachea.
For instance, if a hospital wants to send a patient on a ventilator, he says, “you need to have respiratory therapists and nurses experienced in caring for individuals who require mechanical ventilation, as well as staff who can manage the equipment and safely perform related skills, such as changing tracheostomy tubes, providing tracheostomy care, and suctioning a resident’s trachea.
“When I was a program director at a nursing facility with a ventilator unit in 1990, we had 32 ventilator-dependent residents, and there was always at least one or two respiratory therapists on site, as well as highly experienced nurses,” he says.
If a skilled nursing center wants to take patients with tracheostomy tubes, staff should—at a minimum—know how to properly clean, suction, and change the trach tube, as well as how to monitor for and manage infections or other complications, Horowitz says.
“And, if you admit residents who require mechanical ventilation, it is essential to have a qualified and experienced staff on a 24/7 basis.”
Providers need to validate any education and training have staff received and document it in their personnel record, Horowitz says. He also recommends maintaining sign-in lists for in-service and training programs and keeping the information on file as well. “Apart from the regulatory context, ongoing education, training, and in-servicing is the right thing to do.”
Evans notes that providers need to be practical about how many patients with any condition they can accept. “I’m medical director of a facility that takes patients with trachs. We have 180 beds, but as a practical matter, we can only take about 10 trachs at any given time.”
“This is a time of great uncertainty and little predictability,” Mendelson says. “It’s not a time to take serious risks or to be overly ambitious. I would be cautious about the risk I choose to take. Instead, be proactive about developing strategic partnerships and nurturing them.”
A Changing Marketing Paradigm
Not only are care and staffing needs different for higher-acuity patients, marketing is unique as well. In today’s world, Maun says, “You can’t just send a marketing person to the hospital discharge planner and expect referrals and partnerships. And you can’t hound them for patients you aren’t ready to take.”
“We have specific marketing strategies, and we go to hospitals with our medical directors or other clinical leaders and sit down with discharge planners,” McKenzie says. “We tell them that we are prepared to take patients we couldn’t take before and why we are now able to accommodate this subset of individuals.
“If we aren’t prepared to accept certain kinds of patients,” he says, “it’s not in our best interest to say ‘no’ on the front end. Instead, we say that we will come back to them when we can take those individuals.” If possible, include a time frame—such as three months—when the nursing care center plans to be ready to successfully manage the specific subset of patients.
“When you go back, explain what you implemented to ensure that you can care for those patients. Remind them of your track record with other high-acuity patients, and have data ready to show them,” McKenzie says.
Old Days Are Gone
Watching old TV shows may produce feelings of nostalgia, but yesterday is best left in the past. As Maun says, “Not being willing to change is a death sentence for all business. You can’t wait for the old ways to return—it’s not going to happen.”
Take a deep breath and look forward with confidence.
“You don’t have to snap your fingers and suddenly start taking every patient,” says Maun. “Look at what you have in staffing, expertise, equipment, and services and what the hospital needs. Take the first step now. Once people get on board, you’ll get referrals and partnerships moving, revenue flowing. It gets pretty exciting.”
Joanne Kaldy is a freelance writer and communications consultant based in Harrisburg, Pa.