PDPM Data Trends Part II
Is the COVID-era SNF population CMS is evaluating for a possible parity adjustment the same as the pre-pandemic population?
Daniel Ciolek
4/27/2022
This is the second of a series of articles related to the implementation of PDPM supported by examples of data trends reported by CMS, academic researchers, as well as analyses conducted by AHCA. In this series we will contemplate questions related to patient care delivery, outcomes, and payment model implications informed by observed PDPM data trends. Read Part I.
On October 1, 2019, the Medicare Part A skilled nursing facility (SNF) prospective payment system (PPS) transitioned to the Patient Driven Payment Model (PDPM). In the fiscal year 2022 SNF PPS proposed rule1 and final rule2, CMS proposed but did not implement an approach to apply a parity adjustment intended to assure that total PDPM payments would not be higher than they would have been under RUG-IV.
To rule out impacts of the COVID-19 pandemic, CMS removed SNF claims with a COVID diagnosis and claims related to COVID waivers from their analysis and estimated that PDPM overpaid SNFs in 2020 by 5.0 percent for patients as compared to 2019.
The CMS approach assumes two things. First, the patient acuity composition of the non-COVID/non-waiver patients in 2020 was the same as 2019. Second, that there were no COVID spillover factors that skewed the average PDPM physical therapy (PT), occupational therapy (OT), speech language-pathology (SLP), nursing, and non-therapy ancillary (NTA) component average case-mix index (CMI) rates in 2020. In AHCA comments3, the association supported the general CMS approach. However, AHCA voiced concerns about COVID “spillover” effects and a patient acuity shift in this population that needed mitigation.
This article highlights an AHCA analysis of two PDPM data trends from claims data suggesting that the PDPM data CMS proposed using for its parity adjustment approach in the FY 2022 payment rule is not like the 2019 comparison population, and that COVID “spillover” effects also upwardly skewed PDPM CMIs into 2021.
The red line in the figure provides data trends for SNF Part A admissions between November 2019 and June 2021 after a 3-day qualifying hospital stay that did not have a COVID-19 diagnosis. The blue line shows the shifting PDPM nursing component average CMIs for urban providers during this same period.
Figure: SNF Admission and Nursing Component CMI Trends (Non-COVID/Non-Waiver Claims)
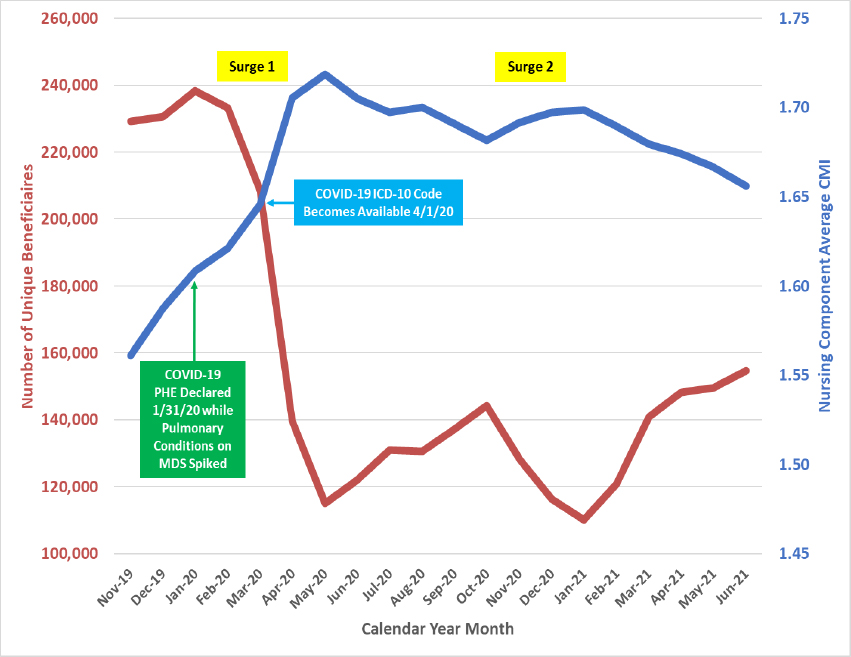
As depicted by the red line, SNF non-COVID admissions from a 3-day inpatient stay dropped over 50% between January and May 2020, with only a partial recovery through June 2021. This corresponds to a suspension of elective surgeries, and a shift to home care for low acuity patients reluctant to enter a SNF, bottoming out as expected during the two COVID surges during this period. It is unclear whether this shift in admission volume and patient acuity mix patterns is temporary, or if it represents a permanent “new normal4,5." Throughout the pandemic, hospitals have been discharging fewer and sicker patients to SNFs than in 2019.
Additionally, the blue line in the chart shows ongoing COVID “spillover” effects elevating CMIs beyond pre-pandemic levels. As depicted by the green box, Nursing CMIs shifted upwards even before the PHE onset. During this period MDS assessments were showing a spike in reported pulmonary conditions, the first COVID cases and deaths in SNFs occurred, and quarantines started. The blue box indicates another upward CMI shift in April when the full force of the pandemic hit. By July 2020, when most patients were vaccinated and COVID cases were lower, the CMIs of non-COVID patients also trended towards pre-pandemic levels but had not stabilized at a “new normal.”
“Spillover” occurs in non-COVID patient CMIs when MDS assessment item patterns change from what would have occurred if not for the pandemic. For example, the pandemic environment of mandatory isolation and visit restrictions resulted in more mood and mental disorders and lower functional mobility reported. These factors significantly impact nursing component CMIs. Notable is that the Nursing component CMIs show an inverse relationship to admission trend, suggesting that during COVID surges hospitals were more reluctant to discharge lower acuity patients to SNFs, increasing the proportion of higher acuity patients. These numbers could approach pre-pandemic levels during an endemic phase of COVID where there is less anxiety and fewer restrictions impacting visitations and mobility. It’s less certain if hospital discharges return to pre-pandemic patterns.
These and similar patterns are important considerations as CMS revisits the necessity of a parity adjustment, and if so, what the adjustment would be. Recently, CMS issued the fiscal year 2023 SNF PPS proposed rule6 attempting to mitigate AHCA’s concerns, primarily by only analyzing months with low COVID prevalence. This revised approach reduced the proposed PDPM parity adjustment from 5.0 to 4.6 percent. While this is a move in the right direction, AHCA will analyze and comment on whether there are remaining unresolved COVID-era “spillover” effects and patient acuity shifts that CMS must account for to avoid a parity adjustment overcorrection that could impact access to care.
Daniel E. Ciolek is the Associate Vice President, Therapy Advocacy at the American Health Care Association.
References
1 86 FR19954, Medicare Program; Prospective Payment System and Consolidated Billing for Skilled Nursing Facilities; Updates to the Quality Reporting Program and Value-Based Purchasing Program for Federal Fiscal Year, 2022, Proposed Rule, April 15, 2021
2 86 FR42424, Medicare Program; Prospective Payment System and Consolidated Billing for Skilled Nursing Facilities; Updates to the Quality Reporting Program and Value-Based Purchasing Program for Federal Fiscal Year 2022; and Technical Correction to Long-Term Care Facilities Physical Environment Requirements, Final Rule, August 4, 2021
3 AHCA Formal Comment Letter Regarding FY 2022 SNF PPS Proposed Rule – CMS-1746-P, Submitted June 4, 2021
4 Medicare Payment Advisory Commission (MedPAC) Report to Congress, Chapter 7, Skilled nursing facility services, March 2022.
5 Brown, D. 2021. A new normal: Experts don't see discharges to SNFs returning to former levels. McKnight's Long Term Care News, April 15.
6 87 FR22720 Medicare Program; Prospective Payment System and Consolidated Billing for Skilled Nursing Facilities; Updates to the Quality Reporting Program and Value-Based Purchasing Program for Federal Fiscal Year 2023; Request for Information on Revising the Requirements for Long-Term Care Facilities to Establish Mandatory Minimum Staffing Levels, Proposed Rule, April 15, 2022.